Epigraph Vol. 21 Issue 3, Summer 2019
Microbiome research in epilepsy: Hope or hype?
The human body, though a miraculous machine, is also a sort of mobile terrarium for other living things. In fact, 99% of the genes in your body aren’t yours – they belong to bacteria, viruses, fungi and other microorganisms. These microorganisms live almost everywhere—in the mouth, eyes, nasal passages, genitals and on the skin—but mostly, they’re in your gut.
The gut microbiome includes hundreds of species of bacteria, comprising 100 trillion cells—more than exist in a human body. Yet until very recently, the idea that these microorganisms could influence human health and behavior was soundly rejected.
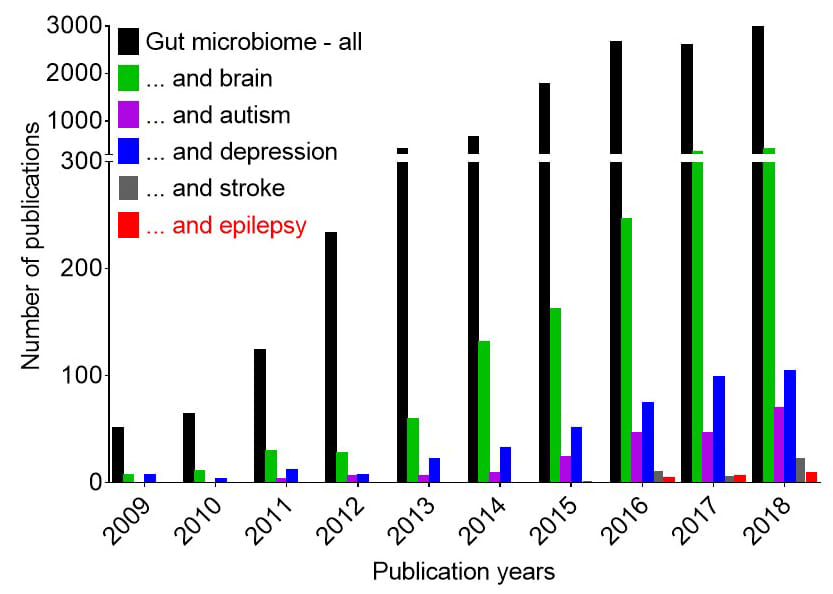
Over the past decade, however, the gut biome has gained some respect (see Figure 1). It’s now recognized as an important part of human health and function, with effects implicated in a variety of conditions, from the obvious (inflammatory bowel disease) to the not-so-obvious (Parkinson’s disease). Neurodevelopmental and mental disorders (such as autism and depression) have been studied most extensively. Neurological disorders, such as stroke and epilepsy, have remained scarcely examined, although interest has been growing.
Figure 1. Publications on the gut microbiome, 2009-2018
The gut-brain axis
Given the blood-brain barrier, the idea that bacteria in the gut could influence the brain was even harder to swallow. But an increasing number of studies are finding intimate communication between the gut and brain, as well as complex interplay among the gut microbiome, the brain and the rest of the body.
Given their range of effects on the body and their constant interactions with the nervous system, gut microbiota are now thought to play a role in many neurological disorders. For example, giving antibiotics to mice prone to Alzheimer’s disease — in order to destroy most of the gut bacteria—reduced the number of clumped proteins in the brain that have been linked with dementia. A later study gave young mice antibiotics for only a week; as they grew, their brains showed less evidence of Alzheimer’s.
Do they play a role in epilepsy? Can gut microbiota affect seizure frequency? Can certain populations of bacteria predispose to seizures, and can we harness the power of the microbiome to stop seizures?
Gut microbiota: The force behind the ketogenic diet
Most research to date is preclinical, but results are intriguing. A landmark study showed that the ketogenic diet alters the gut microbiota across two seizure mouse models, and that changes in the microbiota are necessary and sufficient for conferring the seizure protection of the diet. More specific findings included:
- Gut microbiota is altered by the ketogenic diet and required for protection in the mouse 6-Hz seizure model.
- Mice treated with antibiotics or reared germ free are resistant to the seizure-protective effects of the ketogenic diet.
- Gut microbes modulate seizure susceptibility through mechanisms that do not involve alterations in beta hydroxybutyrate levels (measure of ketosis).
- Diet- and microbiota-dependent seizure protection is associated with elevations in bulk GABA relative to glutamate content in the hippocampus
The gut biome can be altered in many ways, starting even before birth. At birth, delivery by caesarean section results in a different composition of gut biota, compared with vaginal birth. Other factors include infant feeding (breast milk or formula), genetics, infections, diet and medications. In addition to antibiotics, many other medications affect the gut microbiota. A survey of 1,000 medications—including most anti-epileptic drugs—found that 25% of them exerted some effects.
Many of these relationships are bidirectional, with the gut biota affecting predisposition to infections, efficacy of medications and even what people are predisposed to eat (and how much of it they eat). For example, infection with Clostridium difficile is a sign of dysbiosis—a gut biome that is out of balance.
Microbiota affect seizure susceptibility

Transplant studies in rats have provided evidence that the microbiome also may help to modulate seizure susceptibility. Gut biota from chronically stressed rats were transplanted into unstressed rats who had been given antibiotics to deplete their native gut bacteria. After treatment, all rats were subject to kindling of the amygdala to induce seizures. Stressed rats also received gut biota from unstressed rats.
Both stressed rats and the unstressed rats with transplants from stressed rats had seizures sooner, and their seizures lasted longer, compared with controls. Conversely, when stressed animals received gut bacteria from unstressed animals, their seizure susceptibility decreased.
“We showed that if you take an animal that is stressed, and therefore prone to epilepsy, and you give it microbiome samples from a normal animal, those samples exert an antiepileptic effect,” said Andrey Mazarati, professor of pediatrics and neurology at UCLA’s David Geffen School of Medicine and senior author. “It wasn’t preventative, but it normalized the predisposition. This is a potential therapeutic pathway.”
Looking outside the brain box
Quentin Pittman, professor of physiology and pharmacology at the University of Calgary, was one of the reviewers of the original paper. His own research suggests that colitis affects behavior and predisposition to seizures in animals.
“We know that stress changes behavior and changes the properties of the brain, and that it also changes the microbiota,” said Pittman. “Their study raises a lot of questions. What is the mechanism by which the gut biota lead to changes in the brain? Is it a neural link? Do different bacterial groups create metabolites that have effects? Or do they lead to changes in immune cells, which then affect the brain?”
Mazarati and colleagues are now conducting similar tests in a model of post-traumatic epilepsy, while also collecting genomic and metabolomic data. One potential finding is a gut biome signature that could act as a biomarker for the development of epilepsy, or an increased disposition for epilepsy.
“People have been looking for biomarkers but it’s all confined to the brain, or to peripheral markers in the blood,” he said. “We’re going to look outside that box. Only about half of people who experience brain trauma will develop epilepsy, and it can be years later. If we can look at early microbiome changes after trauma, we may see changes that can predict epilepsy farther down the road.”
At this stage, he said, “It is too early to say with certainty whether dysbiosis is indeed involved in epilepsy, and if so, what are mechanisms behind this involvement. Still, several scenarios can be contemplated.”
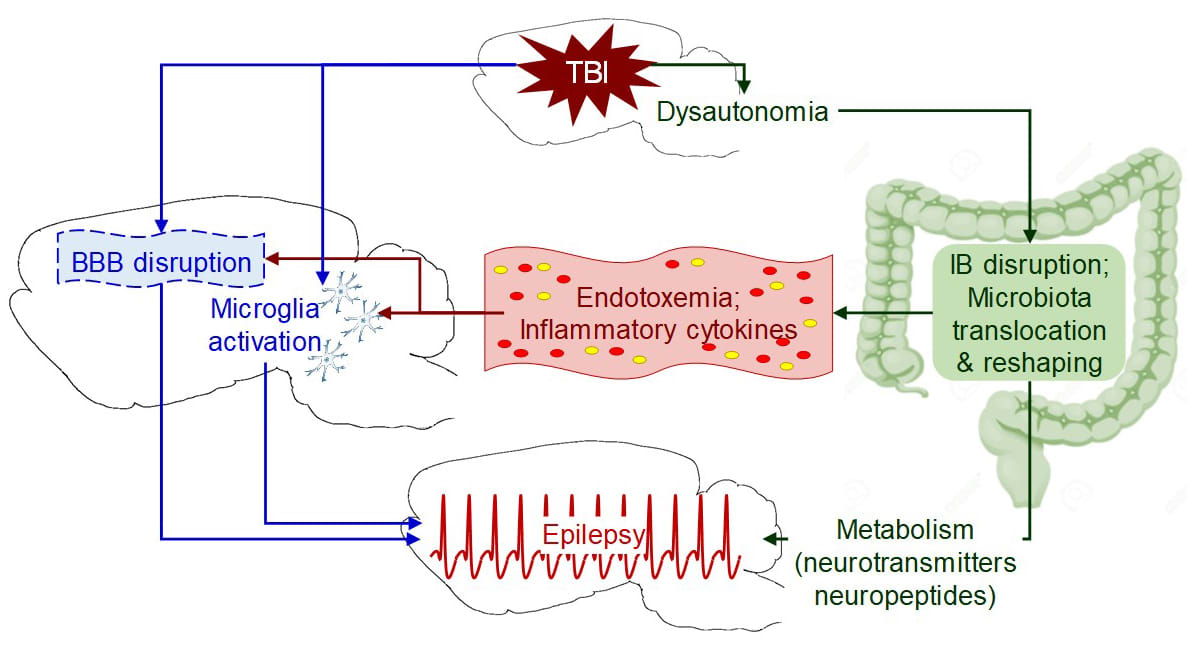
As one example, traumatic brain injury is known to produce abnormal functioning of the autonomic nervous system, with gastrointestinal dysfunction as one manifestation (see Figure 2). This dysfunction includes disruption of the intestinal barrier and changes in gut microbiota composition. These events trigger both peripheral inflammation—the appearance of gut bacterial toxins in blood and a reactive rise in inflammatory molecules such as cytokines—as well as central inflammation (the disruption of the blood-brain barrier and activation of microglial cells). The inflammatory events may promote the pro-epileptic effects of brain trauma, or may themselves precipitate epilepsy.
This link between dysbiosis and epilepsy through inflammation is only one possibility; many metabolic effects of dysbiosis affect molecules that are directly involved in epilepsy, such as neurotransmitters and regulatory neuropeptides.
Figure 2. Hypothetical role of dysbiosis in epileptogenesis after brain injury
Transplanting the gut biome
Studies in other areas have shown the power of transplanting gut bacteria. Fecal transplants can be used to treat infection with Clostridium difficile, with a success rate above 90%.
In epilepsy, only a few transplant case reports exist. One described a fecal transplant given for Crohn’s disease in a patient who also had well-controlled epilepsy (she had a few seizures each year, which seemed to be associated with forgetting to take her medication regularly). After the transplant, she stopped taking anti-seizure drugs and had no seizures for the following 22 months.
Another study documented seizure freedom in six people with drug-resistant epilepsy who were taking antibiotics. After antibiotic treatment ended, their seizures resumed within two weeks.
Finding the right combination
As a less invasive alternative to transplant, introducing probiotics (“good bacteria”) or prebiotics (food for “good bacteria”) to the human gastrointestinal system is another option. Research has found intriguing results in multiple sclerosis, headache and a few other conditions.
Last year, a pilot study in 45 people with drug-resistant epilepsy found that 29% had a clinically significant (>50%) reduction in seizures after 4 months of taking probiotics. However, the study was not placebo controlled.
A recent preclinical study found that probiotic supplements dramatically reduced seizure severity in chemically kindled rats. The supplements also improved learning and memory. Rats given the supplements had decreased levels of nitric oxide and malonedealdehyde—markers of oxidative stress—as well as increased levels of GABA.
The long road to answers
Do people with epilepsy have different populations of bacteria than people without epilepsy? Does successful AED treatment change the gut biota? The answers aren’t known; researchers are still studying what a “normal” gut biome looks like, or if there is such a thing. It may be that gut microbiomes are as distinctive as fingerprints, but it’s more likely they are variations on a theme.
A recent report found differences in the gut biomes of people with drug-resistant epilepsy, compared to those who were responsive to anti-epileptic drugs and healthy controls. The drug-resistant group had more rare bacterial species.
The implications of this finding aren’t clear, studies are beginning to piece together an important role for the gut in the behavior of the brain. “The gut and brain are connected by specific neuronal circuits – they’re not separate entities,” said Mazarati. “We’re using a systemic approach – looking at the organism as a whole, rather than as a bunch of parts. So far, we have very good data.”
Though gut bacteria may be one factor, they aren’t the sole “man behind the curtain” when it comes to epilepsy. Before the gut biome can be integrated as a piece of the epilepsy puzzle, much more research is needed that clarifies how and when gut bacteria exert effects on seizure susceptibility or epileptogenesis.
Subscribe to the ILAE Newsletter
To subscribe, please click on the button below.
Please send me information about ILAE activities and other
information of interest to the epilepsy community