Epigraph Vol. 20 Issue 1, Summer 2018
New AEDs have not improved overall outcomes
An influx of new anti-epilepsy medications has not increased the number of patients who are free from seizures, according to results from a longitudinal cohort study from Scotland.
“Despite the availability of over 15 new drugs, overall seizure control in newly diagnosed patients has not fundamentally changed,” said Patrick Kwan, senior author of the study, which was published in JAMA Neurology.
The study included 1,795 patients (ages 9 to 93) who began initial treatment for epilepsy between 1982 and 2012 at the Epilepsy Center of the Western Infirmary in Glasgow, Scotland. Researchers divided the cohort into three subgroups based on the year each person started AED treatment. All patients were followed for at least 2 years (until 31 October 2014) or until death, whichever came first.

At the end of the study period, 1,144 (64%) had been seizure free for at least the previous 12 months. Most often, seizure freedom was achieved with the first AED prescribed. Seizure freedom rates of the most recent cohort (2002-2012) were not any higher than those of the first cohort (1982-1991).
Despite marked increases in the use of newer AEDs over the study period, both as initial monotherapy and in polytherapy, there was no corresponding increase in seizure freedom rates.
During the first decade of the study, the most commonly prescribed drugs were carbamazepine, valproate and phenytoin. By the final decade, the predominant AEDs were valproate, levetiracetam and lamotrigine.
Among the total cohort of 1,795 patients:
- 46% achieved seizure freedom with the first AED regimen
- 12% achieved it with the second
- 4% achieved it with the third
Among the 1,144 patients who became seizure free:
- 72% achieved seizure freedom with the first AED regimen
- 18% achieved it with the second
- 7% achieved it with the third
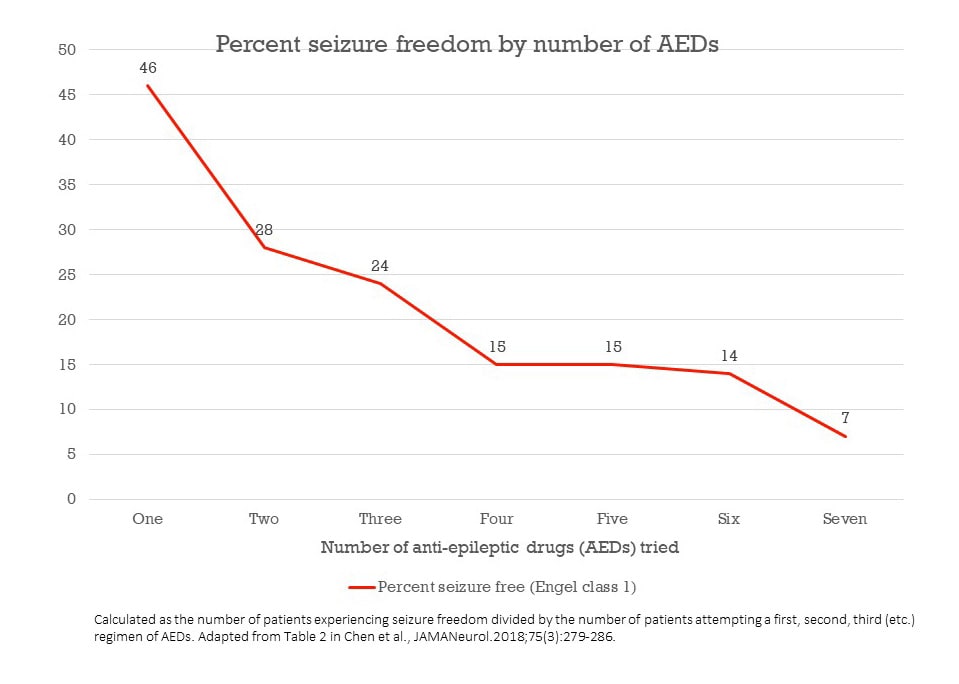
Within each group of patients, the chances of achieving seizure freedom were relatively high for the first three courses of AEDs, but then dropped (see graph).
- 46% of patients who tried one AED regimen (1,795) achieved seizure freedom
- 28% of patients who tried a second regimen (742) achieved seizure freedom
- 24% of patients who tried a third regimen (330) achieved seizure freedom
- 15% of patients who tried a fourth regimen (140) achieved seizure freedom
- 14% of patients who tried a fifth regimen (71) achieved seizure freedom
- 14% of patients who tried a sixth regimen (43) achieved seizure freedom
Ultimately, more than one-third of patients (36%) did not achieve seizure freedom, defined as experiencing no seizures or auras within the previous 12 months.
“We’re not being nihilistic and saying there’s no hope—for individual patients who tried a second and a third [regimen], there is a respectable chance” for seizure freedom, Kwan noted. “But it does get harder after you try two or three drugs.”
Complete seizure freedom, not partial seizure reduction, should be the primary goal, said Martin Brodie, a study author and director of the Glasgow epilepsy center. “Dropping seizure frequency from eight seizures a month to two seizures a month doesn’t improve quality of life,” he said. “Even if you’re only having two seizures a month, you’re always waiting for the next one. You’re wondering when it’s going to happen. The seizure itself almost isn’t even the issue.”

The study illustrates that improving long-term outcomes requires a paradigm shift in treatment and research strategies.
“If we want to make a big difference in seizure freedom, we need to find true anti-epilepsy drugs, not anti-seizure drugs,” said Brodie. “You could say that given the fact we're not actually treating the problem, getting two-thirds of people to be seizure free is pretty good.”
Surgery should be considered if seizures are not controlled after two “well-tried” drugs, said Kwan. “Patients are referred [for surgery] too late—after years of persistent seizures,” he said. “Our center in Melbourne [Australia] recently operated on a woman in her 60s who could have had surgery decades ago. She’s seizure free now—but imagine what her life could have been like. Even in a well-resourced setting like Australia, patients are still referred too late.”
Even if surgery turns out not to be an option, referral to an epilepsy center is crucial, said Jerome Engel, director of the Seizure Disorder Center at UCLA, who was not involved in the study. “Less than 1% of patients who are refractory are referred to epilepsy centers,” he noted. “And it takes an average of 20 years from diagnosis to referral. If a patient is refractory, they deserve to be seen by a team of specialists who can bring everything to bear on why they are continuing to have seizures.”

The results highlight the need for new models, innovative ideas and out-of-the-box thinking from researchers.
“This study’s results show that there’s a population of patients who have something different from what we’re targeting with drugs,” said Engel. “There is a population of patients that requires something entirely different.”
In some cases, people don’t have epilepsy at all: In 20% to 30% of cases, patients with apparent drug-resistant epilepsy who are referred to epilepsy centers are diagnosed with psychogenic nonepileptic seizures (PNES). The delays in referrals translate to years spent living with an incorrect diagnosis.
“It’s valuable that these newer drugs have different side effects because it gives us more to choose from in terms of patient tolerance,” Engel said. “But it’s up to the neuroscientists working in academia to come up with new targets, which would help design truly novel treatments.”
Though several drugs have been approved since the study’s data collection ended in 2012, none of them have made an appreciable difference in seizure treatment, said Brodie.
“We would know right now if we had something better,” he said. “Most of the new drugs work the same way as the old drugs do, or they don’t get people to seizure freedom.”
Kwan agreed. “Patients, their families, and doctors are desperate for new paradigms and novel approaches to treat epilepsy,” he said. “We need new approaches, more adventurous approaches, rather than pouring more money into getting another ‘me-too’ drug out there.”
Subscribe to the ILAE Newsletter
To subscribe, please click on the button below.
Please send me information about ILAE activities and other
information of interest to the epilepsy community