Epigraph Vol. 20 Issue 1, Summer 2018
Proof of concept study aims for rapid genotyping to guide epilepsy treatment
An easy and inexpensive test for the HLA-B*15:02 allele could one day allow clinicians to quickly identify which epilepsy patients are at risk of carbamazepine hypersensitivity, according to study results presented by Gita V. Soraya at the 2018 Asian & Oceanian Epilepsy Congress in Bali.
“This study has provided the proof of principle evidence for the development of a handheld device that can be used at the clinic or bedside for rapid detection of the HLA-B*15:02 allele,” said senior author Patrick Kwan. “This method will avoid the current delay and reduce the cost of testing and make it accessible to patients living in remote areas, allowing carbamazepine to be prescribed more safely.”
Widely used globally as a first-line treatment for epilepsy, carbamazepine also is prescribed for other conditions, such as bipolar disorder and neuralgia.
Carriers of HLA-B*15:02 who take carbamazepine are at high risk for Stevens-Johnson Syndrome or toxic epidermal necrolysis (SJS/TEN). These skin reactions can have an unpredictable course and carry mortality rates of up to 30%.
The allele was first identified in Han Chinese but has since been found in many other Asian populations, including those in Thailand, Malaysia and Hong Kong. The frequency appears lower in India — about 2% to 4% — and is rare in Japan, Korea, and individuals not of Asian descent.
Regulatory agencies, including the U.S. Food and Drug Administration, recommend HLA-B*15:02 screening in patients with Asian ancestry before prescribing. However, because HLA screening is not feasible in most low-resource Asian countries, clinicians avoid prescribing carbamazepine altogether. As a result, patients that could have done well on the drug may receive less effective or more expensive medications.
Soraya noted that the new test has several advantages:
- It uses crude blood samples (no DNA purification needed)
- It requires less blood
- The IDE format requires no labeling or staining of DNA
- Turnaround time is about 80 minutes
- Testing can be completed at the point of care
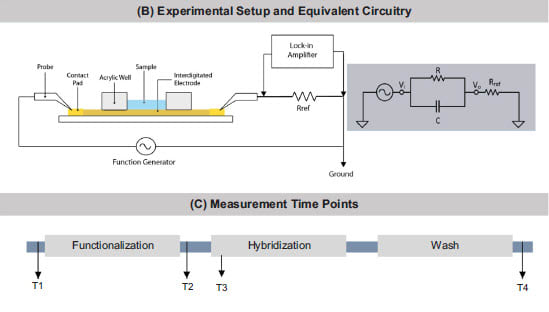
The test is a two-step process. First, HLA alleles are identified and amplified using LAMP. They are then exposed to an interdigitated electrode (IDE) sensor embedded with DNA probes for HLA-B*15:02. If the amplified alleles hybridize with the probes, the electrical impedance of the sensor surface changes, identifying the alleles as HLA-B*15:02.
“The isothermal amplification and electrical-based detection were chosen in order for [the method] to be amenable for miniaturization into a device that can be used at the point of care,” said Soraya, a faculty member at Hasanuddin University, Indonesia.
The study involved a proof-of-concept phase to establish a protocol. Then, the protocol was evaluated for sensitivity and specificity using a sequence of crude blood samples for which the allele type was already known.
The evaluation resulted in one false negative and two false positives, which translates to 92.9% sensitivity and 84.6% specificity.
The false-positive samples differed by only two base pairs (HLA-B*13:01). The HLA-B*13:01 allele also is common in Asian populations but does not appear to confer risk for carbamazepine-induced SJS/TEN. “This must be addressed in future studies,” said Soraya. Subsequent studies also will use larger sample sizes and test more diverse HLA genotypes across various ethnic populations.
Ultimately, she said, “The technology can be customized to detect other alleles relevant in pharmacogenetics testing. It’s also applicable to other gene diagnostics, including pathogen detection.”
The work was undertaken as part of Soraya’s PhD study at the University of Melbourne, Australia, under the joint supervision of Patrick Kwan (Faculty of Medicine) and Stan Skafidas (Faculty of Engineering). Soraya’s presentation was awarded a first-place Tadokoro Prize at the Bali meeting, which attracted more than 1,100 epilepsy specialists from 51 countries. The study was recently published in Biosensors & Bioelectronics.


Subscribe to the ILAE Newsletter
To subscribe, please click on the button below.
Please send me information about ILAE activities and other
information of interest to the epilepsy community