Epigraph Vol. 22 Issue 4, Summer 2020
Setting the record straight on the chances of seizure freedom after two medications fail
A common misperception has spread throughout the epilepsy community: It is said that if the first two anti-seizure medications fail, chances of seizure freedom drop to less than 5%. This is also sometimes reworded as “After two anti-seizure medications fail, the chance of the third failing is 95%.”
Prestigious journals have printed this figure, and respected academics have presented it at conferences. It’s been used in advertisements that promote other epilepsy treatment options, such as nerve stimulation.
It's wrong.
It is true that in Kwan and Brodie’s seminal 2000 study, only 4% of the entire study cohort achieved seizure freedom after two failed medications. And in the 2018 follow-up by Chen et al, only 4.4% of the study cohort became seizure-free on a third medication regimen.
But these percentages are not small because the situation is hopeless—they are small because the study cohort is large. The cohort includes everyone: Those who gained seizure freedom on a first or second medication, as well as those who tried a third medication and anyone lost to follow-up.
Drawing individual-level conclusions using the entire cohort is something like saying “In 2018, there were 3.7 million US high school graduates and 6,000 of them were accepted to the University of X, so the University of X has a 0.16% acceptance rate."
Of course that's not true. Most US high school students didn't even apply to the University of X, so they cannot be included when calculating an acceptance rate.
By the same token, most people in the 2000 and 2018 studies didn’t try a third medication regimen—so they cannot be included when calculating a success rate. The seizure freedom rate for any given medication regimen must include only the patients who tried that regimen, and exclude those who have not.
Such was the main point of a recent letter in Epilepsia, titled “Misperceptions on the chance of seizure freedom with antiseizure medications after two failed trials.”

Authors Benjamin Blond, Lawrence Hirsch and Richard Mattson were compelled to write the letter after years of seeing population-level analysis used to make individual-level claims, culminating with an advertisement falsely stating that “After two anti-seizure medications fail, the chance of the third failing is 95%.”
They note that seizure-free rates after two failed medications are much higher than the misstated 5%. The 2018 follow-up study found that among people who tried a third medication, 23.6% achieved seizure freedom. Similarly, seizure freedom was achieved in 15% of those trying a fourth medication, 14.1% trying a fifth and 14% trying a sixth. (Only 15 people tried more than 6 medications; see table below for data.)

Other research generally aligns with these percentages. In a study of 403 patients, 31% achieved seizure freedom after failing at least two anti-seizure medications. A trial in people with focal epilepsy found seizure-free rates between 11.8% and 17.4% after two failed medications.
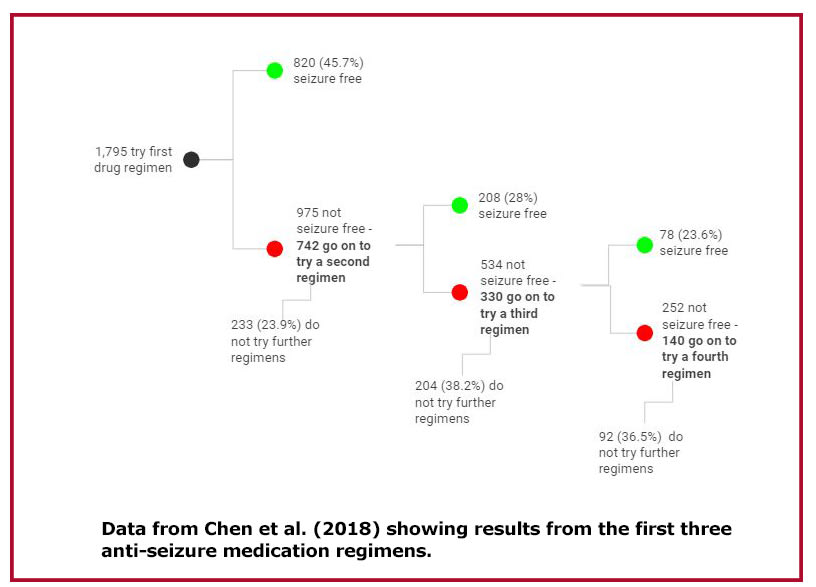
The crucial message for clinicians and patients is that seizure freedom is possible, even if the first two medications don’t work, said Blond, and that conveying accurate seizure freedom rates makes a difference.
“If a patient hears, “’You’ve tried two medications and now you have less than a 5% chance of seizure freedom,’ they might give up,” Blond said. “Not everyone is responsive to the idea of epilepsy surgery and not everyone is a candidate, so where does that leave them? Whereas if they are told there’s a 23% success rate for a third medication, that’s close to 1 in 4 people.”

Kwan agreed with the authors’ assessment. “The letter explains the ‘correct’ method to interpret our data very well,” he said. “At an individual level, the total number of patients who tried a particular regimen would naturally be a more meaningful denominator.”
The goal of the Epilepsia letter was not to discourage people from epilepsy surgery or other treatment options, Blond said, but to help clinicians and patients make decisions using accurate information.
“Seizure freedom makes a huge difference, in terms of quality of life and survival,” Blond said. “If you can help someone achieve that, you can change their life.”
Nancy Volkers
ILAE Communications Officer
Subscribe to the ILAE Newsletter
To subscribe, please click on the button below.
Please send me information about ILAE activities and other
information of interest to the epilepsy community