Epigraph Vol. 22 Issue 4, Summer 2020
Will the pandemic give a permanent boost to telemedicine for epilepsy?
En Español: ¿La pandemia dará un impulso permanente a la telemedicina para la epilepsia?
Telemedicine for epilepsy care is more popular than ever. It has many advantages—but can it sustain itself into the future?
The pandemic pushed many aspects of life online – including health care. Telemedicine has taken hold in many countries as clinics shut down, with non-emergency visits prohibited for weeks.

But telemedicine for epilepsy is far from new. Clinicians around the world have been using it for more than a decade to boost access to care. Whether above the Arctic Circle, in the mountains of Argentina, or in rural areas of the United States, people with epilepsy have benefited from telemedicine programs that bring distant specialty care much closer.
Roberto Caraballo, Juan P. Garrahan Pediatric Hospital, Buenos Aires, has worked for years to establish a telemedicine program in Argentina’s province of Tucuman. With support from the Ministry of Health, the program links Juan P. Garrahan with hospitals in San Miguel de Tucuman and the outlying towns of Tali del Valle and Concepcion. A secure internet connection allows for synchronous audio and video between patients and physicians.
Saving money and time
Before the program, rural families with an appointment in San Miguel de Tucuman had to set aside most of a day and coordinate (and pay for) four bus rides and two taxis.
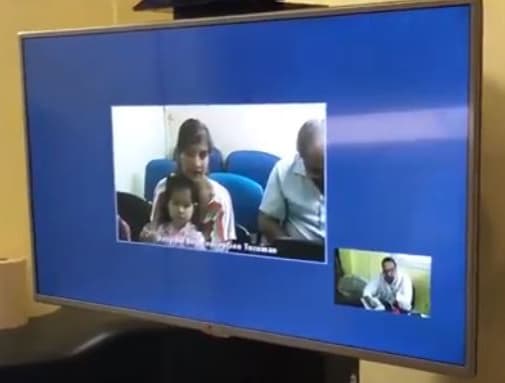
Once the telemedicine program was established, families needed only to get to Tali del Valle or Concepcion, where they see their physician using the local hospital’s telemedicine equipment. A 2019 survey of 116 parents found that 100% felt supported by the clinical teams. Compared with usual care, parents reported that telemedicine led to less lost time from school and work, fewer travel-related costs, better access to medication, and more regular follow-up visits. Listen to families talk about how the telemedicine program has helped them / Escuchar a las familias hablar sobre cómo el programa de telemedicina les ha ayudado.
Though the United States is a high-income country with robust systems of health care, rural areas lack epilepsy specialists. For example, 69% of counties in the state of Michigan are considered medically underserved, and large areas of the state have limited access to pediatric neurologists. A three-year grant established a state program to use telemedicine for pediatric epilepsy, including transition of care from pediatric to adult neurologists. Patient satisfaction was 100%, and physician satisfaction 97%.
Other US rural areas also are being served through telemedicine programs, such as the Cleveland Clinic’s Project IMPACTT, which expects to improve continuity of care and save families at least US$600 per visit. In addition to providing televisits, the project has established online support groups and epilepsy education programs, including a series of free webinars.
Epilepsy care at the North Pole
At the turn of the 21st century, Nizam Ahmed was the only epileptologist in the Canadian province of Manitoba. When he moved west to Edmonton, Alberta in 2002, some of his Manitoban patients wanted to continue seeing him.

“They started driving or flying to Edmonton,” he said—a distance of 1,000 kilometers or more. “There were travel costs, plus the time, plus escort time—because of their seizures they could not drive, so someone else had to come along. Each visit took a few days and so much money.”
So Ahmed gave telemedicine a try, connecting Edmonton with a clinic in Manitoba, where his patients went to “see” him virtually.
“This was 2002 or 2003, so we did not have fancy equipment,” he said. “The audio and video were choppy and not synched up, but we persevered, and patients were so thankful.”
It started him thinking. If he could care for patients in Manitoba while sitting in Edmonton, couldn’t he care for patients in other areas of Canada? Such as, for instance, the North Pole?
Well, not exactly the North Pole, but above the Arctic Circle on King William Island, in a town called Uqsuqtuuq (or Gjoa Haven). If you live there and travel to Edmonton for epilepsy care, each office costs more than a roundtrip flight to Europe. With telemedicine, patients in Uqusuqtuuq need only to walk to the nursing station in town.
Aligning access to patients
Ahmed’s feasibility study was one of the first published on telemedicine for epilepsy. The 2008 report showed that telemedicine, on average, saved each patient more than CD $400 per visit. It also saved time; with conventional office visits, 60% of patients missed more than 5 hours of work, and 90% of them required escorts, many of whom also missed work.
Patients were so grateful for the telemedicine option that some offered to help Ahmed pay for it if program grants didn’t come through. They did, however, and the program is still running; Ahmed estimates he has seen thousands of patients through telemedicine. He also helped to start an epilepsy surgery program in Pakistan through telemedicine; after two years of teleconferences and online counseling visits with patients, Ahmed and colleague William Boling traveled to Pakistan to conduct the first surgeries.
“When you can do it at the North Pole, you can do it anywhere,” he said.
Epilepsy care as conversation
Ongoing epilepsy care may be particularly well suited to telemedicine, noted Samuel Wiebe, University of Calgary. “Most of a follow-up visit is a conversation,” he said. “How many seizures have you had, what happened during them, when were they, are you taking your medications, how is your depression. Epilepsy is a specialty for which we can really go virtual.”
Wiebe estimated that at the height of the pandemic in Canada, 95% of his patient visits were done by phone. Patients appreciated the switch, as it allowed for continuity of care while also saving on time, effort and costs.
There are advantages for the clinician as well. “The visits are more productive because I can look at their information while I’m talking to them on the phone,” he said. “In a face-to-face visit, that’s not good human interaction. People also understand that in a phone call, I have only so much time to talk.”
Advantages of the home environment

At Hospital Universitario de San José Infantil and Instituto Roosevelt in Bogotá, Colombia, J. Sebastian Ortiz de la Rosa now sees his pediatric patients and their families through video calls. “People are happy with this approach because normally, they would spend the whole day coming to the office and waiting,” he said. “Now they’re scheduled at a certain time, a window pops up, and we talk.”
Ortiz de la Rosa appreciates seeing his young patients in their homes. “When kids come into my exam room, they are often shy—they don’t want to talk to me,” he said. “But when they’re at home, I can see them acting naturally. That gives better information, especially for kids with cognitive impairment issues.”
In Japan, telemedicine was first deemed acceptable for outpatient visits in April 2018, though the nationalized health care system capped its use at 10% of patients and required face-to-face visits for each patient at least every 3 months.
When the COVID-19 pandemic erupted, the Japanese Ministry of Health expanded the use of telemedicine, said Akio Ikeda, Kyoto School of Medicine. Though still considered temporary, telemedicine is now widely used for outpatient clinics and generally well accepted.
Pre-pandemic, Nathalie Jetté rarely used telemedicine with her patients at Mt. Sinai Hospital in New York. Now she sees nearly all patients this way and estimates that her department’s use of telemedicine has increased more than 5,000%.
Jetté employs mostly video visits, with the occasional phone conversation or use of an app. “Video visits in particular have allowed me to see my patients in their usual environment, which has enhanced my understanding of their daily lives,” she said. “It also has allowed my patients to have their family members or friends join calls, which helps me provide epilepsy education. It has facilitated multidisciplinary visits as well, as multiple providers can participate in a single visit.”
With no need to juggle exam room space, virtual visits also are more easily scheduled—and people are more likely to show. Patients have been overwhelmingly positive about the change, said Jetté, with many requesting to continue televisits after the pandemic subsides.
Limitations: Bandwidth, reimbursement, literacy
Not every region has employed telemedicine. In south Iran, the modality remains nonexistent despite the pandemic. “there was no infrastructure, rules or policies, or reimbursement process for telemedicine,” said Ali Asadi-Pooya, Shiraz University of Medical Sciences. He does not see telemedicine taking hold any time soon—and that concerns him, as patients unwilling to visit a clinic or hospital are not being seen.

Emanuel Sanya, a neurologist with Nigeria’s University of Ilorin, has seen more educational webinars since the pandemic began, as well as the establishment of call-in services for medication refills. However, telemedicine visits have been largely thwarted in Nigeria and across sub-Saharan Africa, due to the high cost and low availability of internet access. Spotty electricity supplies, lack of access to smartphones, and patient illiteracy are also major barriers.
Juan Carlos Perez-Poveda, San Ignacio University Hospital, Bogotá, noted that overall, one-third of the population of Latin America has no internet access, and access is lower in most individual countries; for example, in Colombia, 42% of the population has no internet access. “Another barrier is that not all hospital care centers have the systems and technologies” necessary to participate in telemedicine, he said.
While the pandemic spurred some positive changes in reimbursement for telemedicine, some health systems are not providing sustainable remuneration and others have begun to pull back from full reimbursement.
“This is the time to think seriously and put some pressure on to ensure that if physicians are providing a service, regardless of the mode, they will be appropriately compensated,” said Ahmed. “If we’re all on board, change has to come on a provincial or state or national level.”
Improving access to care requires change
Many lower-income and older patients may not have the technology or skills to participate in video calls. One US-based insurance plan for older Americans (65 and older) found that one-third of its members didn’t own a computer, tablet or smartphone. In addition, almost 40% had vision issues and 28% had hearing impairments, which could affect communication during virtual visits.
Older physicians, too, may be less willing to “see” patients virtually. “Some of my older teachers hate [the shift to virtual care],” said Ortiz de la Rosa. “They say, ‘No, you need to get to the patient and touch the patient.’”
But with EEG and imaging available online, as well as seizure videos and patient history, he said, telemedicine has robust capability for delivering epilepsy care. And virtual adaptations to other tests and procedures are developed all the time.
“There’s a lens for your mobile phone that can be used to perform a virtual fundoscopy,” said Ortiz de la Rosa. “If you can have one of those in one clinic in a rural area, then you can have most of the things you’ll need to do a proper neurological consult” – without ever being in the same room with the patient.”
Despite some limitations, virtual visits can provide an excellent opportunity to expand access to care in low- and middle-income countries.
“With the old-school ways of doing medicine face to face, people who are far away from cities cannot get the treatment they need because they cannot afford to travel for it,” said Ortiz de la Rosa. “If you can have one computer in the middle of the Amazon rainforest, you are solving problems that otherwise couldn’t be solved.”
Ahmed also is hopeful that the telemedicine trend will take hold more generally.
"The pandemic has helped us to move from rituals to essentials," he said. "A lot of rituals are done in clinic: Non-essential information is collected; non-essential exams are done. With the pandemic, we were forced to pare it down to the essentials. Once people got a taste of that, they realized we should have done it years ago."
The lasting acceptance of telemedicine requires policy changes to allow for coverage and reimbursement, said Ahmed. It also requires physician flexibility. “You have to convert to technology,” he said. “If you don’t believe it can work, it will still eventually come, but it will be forced upon you.”
Nancy Volkers
ILAE Communications Officer
Subscribe to the ILAE Newsletter
To subscribe, please click on the button below.
Please send me information about ILAE activities and other
information of interest to the epilepsy community